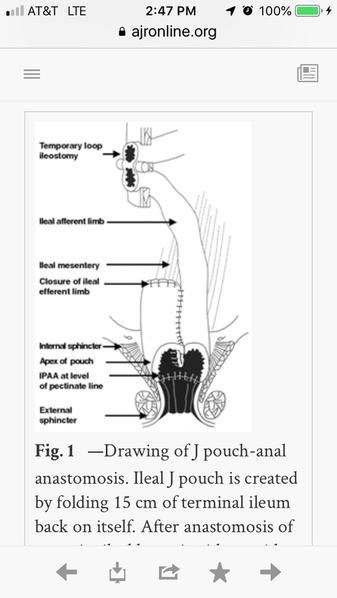
ok, so the intestine is looped back on itself forming a J. The bottom of the curve is cut so it forms a new opening. My question is: is there still tissue in between the sides of the pouch? if I were to insert two fingers, would one finger be in one side of the pouch and the other in the other, or is the middle "cut out" so it's one big true pouch?
Replies sorted oldest to newest
Not that I want any fingers in there. It's just the best way I could imagine posing the question to show what I was asking.
Hi cajundoc. According to Wikipedia, the inner walls are removed to form the pouch. Good question. I certainly didn't know.
Aimee
Yes, the j pouch is a true pouch. It is hollow inside. When your small intestine was looped to form a "J" an instrument was inserted into the "cut end" (the bottom of the loop that is sewn to your anus). The instrument looks like a long staple gun and it staples your loop together permanently. While stapling, this same instrument also cuts the piece of middle tissue so that your loop is now a hollow pouch. I asked my surgeon, he said it is definitely hollow, and he drew a picture for me. There is also a YouTube video of an actual surgery removing the colon (for real) and constructing the j pouch, showing the staple gun making the cut. You need a strong stomach to watch.
Can you post the link? My entire surgery was videoed. Very strong stomach here.
Hi, Cajundoc. I searched for a post I made here in 2016 with the video attached but couldn't find it on this site. If you go on YouTube and search for "IMEDEX, Understanding the techniques of a colectomy with an ostomy and j pouch" you will find the video. There are several IMEDEX surgery videos so look for the one that is 22:19 minutes long. It shows a surgeon lecturing on a j pouch creation and stapling the pouch. Warning: it is graphic so if anyone is waiting for their surgery, please be aware.
Thank you for this topic, the video and explanations. I'm always interested in the physiology of the j-pouch and I wondered the same thing. This topic has helped.
Attachments
The inside of the pouch is an open reservoir. Like a balloon. The seam, or stitching, seen in your posted diagram is only to show where the two limbs were stapled together. If the pouch was two separate limbs stapled together the stool would fill up only in one limb before you feel pressure to go to the toilet. What would be the use of the other limb? Ask your surgeon at your next appointment if the pouch is hollow, or stapled into two separate limbs. Or, Google for real images of the inside of a j pouch. You will see "owl's eyes" at the top (the view of the camera looking into the pouch via the anus) and an empty, hollow chamber that is the pouch. No stitching or stapled tissue. Not separate limbs. It took me a while to understand this concept, but it makes perfect sense, and my surgeon confirmed this. He has created hundreds of pouches in his long career.
I figured as much and googled dozens of time but the images always showed the exterior surface of the staples pouch. I’ll google the owls eye. I’m also a wildlife rehabber and have seen many owls eyes. I’ll look for a comparison!
I asked my surgeon. They said they staple the intestine for form a J and at first there is indeed a septum but as they staple it they cut the septum out and sew it to a true pouch so it holds more stool.
Good post and replies, everyone. THANKS!
My pouch just seems small. Thanks for the replies, people! I wish the biologics were around back in the days of my UC. Also, I have to use the toilet about 5 times a night. What about you?
I do not eat anything past 6 pm and am usually able to make it through the night without going.
WOW. I haven’t had a full night’s sleep in 21 years!
One week post take down I go 1-2 times per night
I’m kinda baffled. I would pay 1000 bucks to just go twice in a night. My sleep suffers terribly. I think my pouch is just smaller. Things may have progressed since mine 22 years ago.
Cajun, I had mine in 1986. At THAT time they didn't leave all the nerve endings inside the rectal cuff, and so I'm totally incontinent at night. I have always worn an Always pad with wings all night and all day too, but of leakage. I wake up about 3-4 times a night and have to go a little bit. But I just keep myself quiet, don't fret about it and fall right back to sleep. It is possible. That's always the way it is for me, so not a big deal. You COULD have a small pouch, OR it could be you haven't stretched it out. Try to hold it in just a little bit longer during the day (wear some protection just in case) and it will stretch. Also, don't eat 4 hrs. before you go to bed, don't eat processed and fried foods. Those go thru your system faster, and it's not good for us to eat that stuff. Hope that helps a bit.
Thank you!!! I do eat late at night. I’m just so hungry all the time. I’ll take your advice and try it though! Thanks!!
That's definitely the problem, and WHAT you eat. If you're eating processed junk food, that will definitely cause a problem. Probably not hungry, just habit. Drink water!
We’ve strayed from the original topic, but getting a good night’s sleep is a big deal. This has been posted about frequently, so a search of past posts will yield a wealth of ideas. I’m lucky enough to have been able to work out ways to sleep through the night just about every time.
1) Do you have untreated (or inadequately treated) pouchitis? That’s the most important thing.
2) A bowel slower (Imodium or Lomotil) at bedtime can be very helpful, *especially* if it’s not used during the day. Lomotil works best for me, and 1 tablet seems sufficient.
3) Stop eating a few hours (or more) before bedtime.
4) A very small fatty meal (like a spoonful of peanut butter) at bedtime helps some people a lot.
5) Soluble fiber at dinner time (e.g. psyllium) can thicken things up and for some people reduce leakage and accidents.
6) If you’re using a sleep aid you might be more likely to miss the signals that your pouch is getting busy.
7) Have you taken the time to “stretch your pouch” (i.e. increase its capacity)? Some of us were advised to do this after surgery, by delaying bathroom visits (during the day) to gradually increase tolerance for a not-quite-full pouch. I still do this years later, though in a less structured way. Unless I’m going out I try not to use the toilet prematurely, and it feels like a useful challenge to pee without pooping when my pouch is half- or three-quarters-full.
8) On the occasions when I do wake up with a sensation of pouch fullness I sometimes choose to go back to sleep anyway. This is tricky to get right, of course, but it seems to help remind my body that my pouch doesn’t always need to be emptied just because I have a sensation.
9) Patiently empty your pouch at bedtime. Anything left in there is an alarm clock set to the wrong time.
Good luck!
I had my surgery in 1985. I had to fill my pouch with water three times per day to stretch it out prior to takedown. Not sure if they still do this. But I'm thinking this is one reason I am able to sleep through the night. Also kegal exercises. I have never had an accident.
Excellent info, Scott. Thanks! That can sure help. Accept it: I wonder if they left your nerve endings in place and that is also the reason for your good fortune. I stretched it out and did kegals also, but always have leaked at night.
Some folks have had smoldering, untreated pouchitis for many years. It can be completely responsible for chronic nighttime leakage or interrupted sleep. A simple course of an appropriate antibiotic is life-changing in these cases.
It seems Flagyl and Cipro are the 2 antibiotics that help, yes?
Scott F posted:Some folks have had smoldering, untreated pouchitis for many years.
I should note that I have had “smoldering” Pouchitis WITH treatment for around 25 years. Remicade and rotating antibiotics have kept me in this state and one can have a good quality of life in this state so long as the inflammation is reasonably kept in check.
My most recent scope done on May 22, 2019 showed what has been a recurring pattern of inflammation in 3 areas- the rectal cuff, the Pouch inlet and the neoterminal ileum. I think a pattern of inflammation at the Pouch inlet is fairly common due to backsplash stool as a result of there being no backsplash valve at the inlet, as there is in the colon. My actual J Pouch interior looks really good- it’s just the above 3 hot zones that have inflammation that is mild and scattered.
My doctor noted the strength of my anal sphincter. He said a lot of people have leakage issues as they get older with pouches but that’s not happened to me so far. It got 20 years of great exercise with ulcerative colitis and I believed I really toned it up during that period, having to constantly stave off the wild urge to defecate.
does anyone know what causes pouchitis and how to avoid it?
The cause of pouchitis is uncertain, though various theories exist. There are two ways to prevent or delay it that *sometimes* work: substantial doses of bacterial probiotics (VSL #3, now called Visbiome, is the one that’s been properly tested), and very-low carbohydrate diets. All carbohydrates are the same for this purpose, so starches, fruit, sugar, etc. are all equivalent carbs, and all need to be reduced for this diet. Calling some carbs “healthy” doesn’t change the fact that they are carbs. It’s a tough diet, I think, and it doesn’t work for everyone.
Cipro and/or Flagyl are the most common first-line pouchitis meds. Some doctors use Xifaxan/rifaximin, but I think it probably doesn’t work as well. When one doesn’t work or causes bad side effects another one may be effective and well-tolerated.
”Smoldering” can mean different things to different people. I intended it to mean a relatively mild case of pouchitis that causes some nighttime leakage or awakening, but doesn’t get worse than that. If it causes no symptoms at all but some inflammation can be seen on pouchoscopy I’d tend to call that “subclinical pouchitis.” There’s nothing inaccurate about calling such a case “smoldering,” but it makes two very different situations sound the same.
Does taking visbiome or any other probiotic mean that we can have more carbs? Or are we speaking about taking visbiome a and not having carbs as well or cutting back on carbs. What I'm trying to say is when we are taking a probiotic will that help with the carb intake?
no real Correlation here
CT , you mentioned the various types of low level chronic inflammation. Does that cause burning or any pain during defecation? I’ve had cuffitis and Pouchitis (not continuously but mostly) since takedown 18 months ago. I still burn with a bm but not afterwards like I used to.
I have no burning or pain during defecation, but closer to takedown I did. The reason you are having that sensation is that it takes a while for the pH level of the stool to adjust after takedown. I may have had that for up to 2 years after takedown. It has nothing to do with inflammation and everything to do with pH of stool. Butt burn is for the same reason. The stools are too alkaline and this changes over the course of time as your body adapts.
There’s no clear connection between low carbs and probiotics. Not everyone benefits from either intervention, and some people benefit more from both than from one. These are fuzzy interventions that are tricky to evaluate, requiring patience, consistency, and objectivity, and they don’t tend to completely eliminate episodes of pouchitis, nor are they likely to completely eliminate the need for more definitive treatments (e.g. courses of antibiotics periodically). They may reduce that need.
That being said, if probiotics are more tolerable for you than a very low carb diet then it’s probably better to try probiotics first, and get aggressive with them before considering the diet change. It’s also okay to choose a more liberal diet and accept the possibility (not certainty) of a more frequent need for antibiotics. *All* of this is intended to help you feel and function better, so your preferences matter a lot.